In idiopathic TTP, severely decreased (<5% of normal) ADAMTS13 activity can be detected in most (80%) people, and inhibitors are often found in this subgroup (44–56%). Hence, without proper cleavage of vWF by ADAMTS13, coagulation occurs at a higher rate, especially in the microvasculature, part of the blood vessel system where vWF is most active due to high shear stress. Very large vWF multimers are more prone to lead to coagulation. ĪDAMTS13 is a metalloproteinase responsible for the breakdown of von Willebrand factor (vWF), a protein that links platelets, blood clots, and the blood vessel wall in the process of blood coagulation. These cases are now classed as an autoimmune disease and are known as autoimmune TTP (not to be confused with immune/idiopathic thrombocytopenic purpura). The relationship of reduced ADAMTS13 to the pathogenesis of TTP is known as the Furlan-Tsai hypothesis, after the two independent groups of researchers who published their research in the same issue of the New England Journal of Medicine. TTP of unknown cause was long known as idiopathic TTP but in 1998 the majority of cases were shown to be caused by the inhibition of the enzyme ADAMTS13 by antibodies. Not to be confused with Immune thrombocytopenic purpura. The majority of the remaining cases are secondary to some other factor. The two best understood causes of TTP are due to autoimmunity and an inherited deficiency of ADAMTS13 (known as the Upshaw-Schülman syndrome). These platelet-vWF complexes form small blood clots which circulate in the blood vessels and cause shearing of red blood cells, resulting in their rupture and formation of schistocytes. Platelets are consumed in the aggregation process and bind vWF. TTP, as with other microangiopathic hemolytic anemias (MAHAs), is caused by spontaneous aggregation of platelets and activation of coagulation in the small blood vessels. High blood pressure ( hypertension) may be found on examination. Hemolytic anemia ( microangiopathic hemolytic anemia).The classic presentation of TTP, which occurs in less than 10% of people, includes five medical signs. Larger bruises ( ecchymoses) may also develop. 
The bruising often takes the form of purpura, while the most common site of bleeding, if it occurs, is from the nose or gums. As a result, bruising, and rarely bleeding can occur. Īs TTP progresses, blood clots form within small blood vessels (microvasculature), and platelets (clotting cells) are consumed. Other symptoms include, but are not limited to jaundice or paleness of the skin, a fast heart rate or shortness of breath, or pinpoint-sized purple or reddish dots on the skin known as petechiae. Seizures and symptoms similar to those of a stroke can also be seen. Frequently reported symptoms include feeling very tired, confusion, and headaches. Neurological symptoms are very common and vary greatly in severity. Many people experience an influenza-like or diarrheal illness before developing TTP. The signs and symptoms of TTP may at first be subtle and nonspecific. The underlying mechanism was determined in the 1980s and 1990s. The condition was first described by Eli Moschcowitz in 1924. Onset is typically in adulthood and women are more often affected. Platelet transfusions are generally not recommended. Immunosuppressants, such as glucocorticoids, and rituximab may also be used. With plasma exchange the risk of death has decreased from more than 90% to less than 20%. It may be supported by measuring activity of or antibodies against ADAMTS13. Diagnosis is typically based on symptoms and blood tests. Less commonly TTP is inherited, known as Upshaw–Schulman syndrome, such that ADAMTS13 dysfunction is present from birth. This results in decreased break down of large multimers of von Willebrand factor (vWF) into smaller units. The underlying mechanism typically involves antibodies inhibiting the enzyme ADAMTS13. Known triggers include bacterial infections, certain medications, autoimmune diseases such as lupus, and pregnancy. In about half of cases a trigger is identified, while in the remainder the cause remains unknown. Symptoms may include large bruises, fever, weakness, shortness of breath, confusion, and headache. This results in a low platelet count, low red blood cells due to their breakdown, and often kidney, heart, and brain dysfunction. Thrombotic thrombocytopenic purpura ( TTP) is a blood disorder that results in blood clots forming in small blood vessels throughout the body. Hemolytic-uremic syndrome (HUS), atypical hemolytic uremic syndrome (aHUS) 
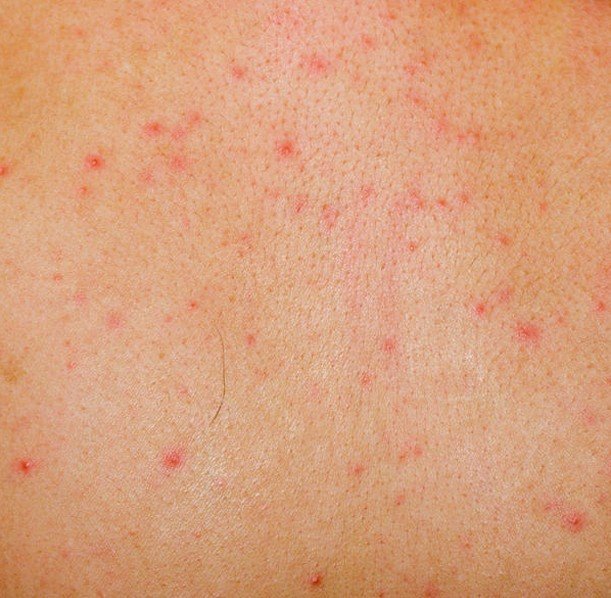
Unknown, bacterial infections, certain medications, autoimmune diseases, pregnancy Large bruises, fever, weakness, shortness of breath, confusion, headache Spontaneous bruising in a woman with critically low platelets Moschcowitz syndrome, idiopathic thrombotic thrombocytopenic purpura 
Medical condition Thrombotic thrombocytopenic purpura
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
